|
Enrolled patients were randomly assigned 1:1 in blocks of four per stratum to receive pembrolizumab 200 mg every 3 weeks for up to 35 cycles or the investigator's choice of platinum-based chemotherapy for four to six cycles. 
Randomisation was computer generated, accessed via an interactive voice-response and integrated web-response system, and stratified by region of enrolment (east Asia vs rest of world), ECOG performance status score (0 vs 1), histology (squamous vs non-squamous), and PD-L1 TPS (>= 50% vs 1-49%). Eligible patients were adults (>= 18 years) with previously untreated locally advanced or metastatic non-small-cell lung cancer without a sensitising EGFR mutation or ALK translocation and with an Eastern Cooperative Oncology Group (ECOG) performance status score of 0 or 1, life expectancy 3 months or longer, and a PD-L1 TPS of 1% or greater. Methods This randomised, open-label, phase 3 study was done in 213 medical centres in 32 countries. We investigated overall survival after treatment with pembrolizumab monotherapy in patients with a PD-L1 TPS of 1% or greater. 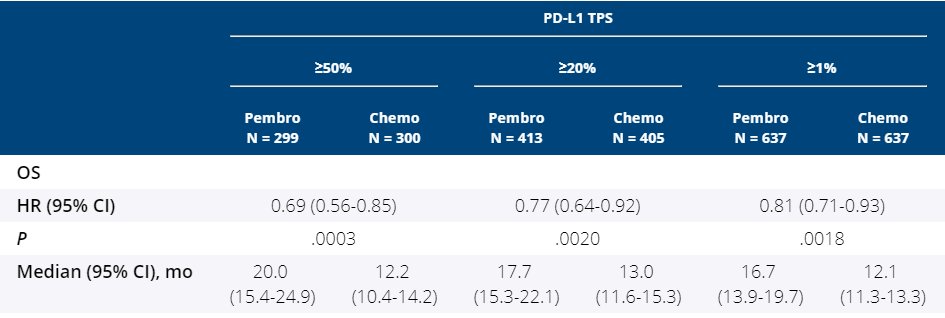
LANCET, v.393, n.10183, p.1819-1830, 2019īackground First-line pembrolizumab monotherapy improves overall and progression-free survival in patients with untreated metastatic non-small-cell lung cancer with a programmed death ligand 1 (PD-L1) tumour proportion score (TPS) of 50% or greater. BONDARENKO, Igor KUBOTA, Kaoru LUBINIECKI, Gregory M. CASTRO JR., Gilberto SRIMUNINNIMIT, Vichien LAKTIONOV, Konstantin K. WU, Yi-Long KUDABA, Iveta KOWALSKI, Dariusz M. Pembrolizumab versus chemotherapy for previously untreated, PD-L1-expressing, locally advanced or metastatic non-small-cell lung cancer (KEYNOTE-042): a randomised, open-label, controlled, phase 3 trial These data confirm and potentially extend the role of pembro monotherapy as a standard first-line treatment for PD-L1-expressing advanced/metastatic NSCLC.Please use this identifier to cite or link to this item: Conclusion: KEYNOTE-042 is the first study with a primary end-point of OS to demonstrate superiority of pembro over platinum-based chemo in pts with previously untreated advanced/metastatic NSCLC without sensitizing EGFR or ALK alterations and a PD-L1 TPS ≥1%. The external DMC recommended continuing the trial to evaluate PFS (secondary end-point). Grade 3-5 drug-related AEs were less frequent with pembro (17.8% vs 41.0%). Pembro significantly improved OS in pts with TPS ≥50% (HR 0.69), TPS ≥20% (HR 0.77), and TPS ≥1% (HR 0.81) (Table). After 12.8-mo median follow-up, 13.7% were still on pembro and 4.9% were receiving peme maintenance. Results: 1274 pts were randomized: 637 to each arm. Efficacy boundaries at the prespecified second interim analysis were one-sided P =. 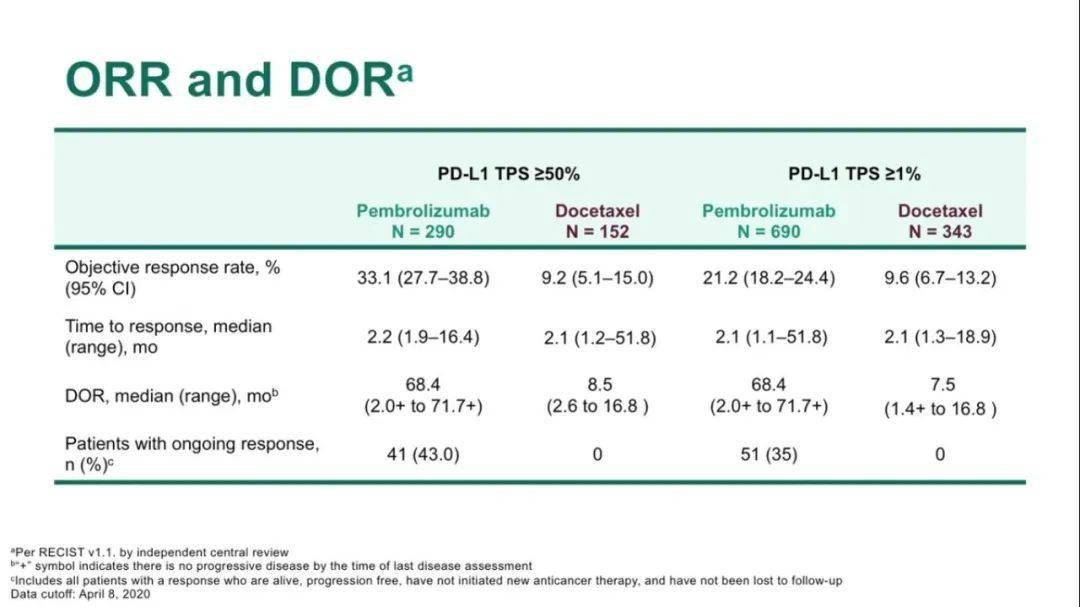
OS differences were assessed sequentially using the stratified log-rank test. Primary end-points were OS in pts with TPS ≥50%, ≥20%, and ≥1%. Randomization was stratified by region (east Asia vs non-east Asia), ECOG PS (0 vs 1), histology (squamous vs nonsquamous), and TPS (≥50% vs 1-49%). Methods: Eligible patients (pts) were randomized 1:1 to ≤35 cycles of pembro 200 mg Q3W or investigator’s choice of ≤6 cycles of paclitaxel + carboplatin or pemetrexed (peme) + carboplatin with optional peme maintenance (nonsquamous only). In KEYNOTE-042, we compared pembro with chemo at the lower TPS of ≥1% (NCT02220894). Background: In KEYNOTE-024, pembro significantly improved PFS (primary end point) and OS (secondary end-point) over chemo as first-line therapy for metastatic NSCLC without targetable alterations and PD-L1 TPS ≥50%.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
